Did you know that PPE is actually the very last level of infection control??? To be honest, I have to admit that I had NO IDEA. Until COVID-19 became the impetus for my increase in research and writing, I had no idea that people other than healthcare professionals and their governing bodies were making an effort to reduce infection. And, I’m not commenting on everyone washing their hands or our sterilization teams (whom I consider to be in the group of healthcare professionals). I mean there are construction workers, HVAC people, contractors, architects, builders, and entire governing bodies that don’t work in patient care that do 85% of the work of infection control. Let’s call them out!
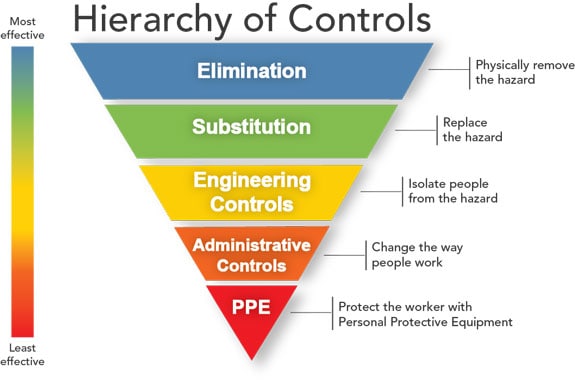
The infection control process is actually best illustrated as an upside down pyramid. Once you read through it, you will say to yourself, “Well, of course! I knew that!” But you didn’t really think of it until now, did you? There is actually an entire initiative dedicated to Prevention through Design! If you take a look at how this pyramid is constructed, you can see the levels of effectiveness are right alongside the intervention. And guess what? PPE is the LEAST effective method of infection prevention for patients and for healthcare workers. There is a link on the Resources page that will take you to the NIOSH document for infection prevention controls for more details about how some of these things are done.
I’m going to go through each of these steps to explain and give you an example of how this works. I’m going to use the hazard of stairs as my primary example. Obviously not an infection but may of these steps can’t apply to infection, which is why we need so many steps! But, they can all apply to stairs. Then we will go back and talk about infection control.
Elimination. If only it were this easy, right? Let’s just eliminate the hazard and then we don’t have to deal with it anymore. We all know it is never actually that easy. The flu can’t be eliminated so matter what we try. But there are some instances where elimination can work. Eliminate stairs from a hospital and you don’t have to worry about anyone falling down them. Keep everything on one level and no problems from stairs will arise. Obviously this can’t always be done, especially if the building has already been built, and we are trying to reduce the falls down the stairs 10 years later. That’s why there is another step…
Substitution. So instead of stairs, we can have elevators! Of course this isn’t a full substitution because we still have to have stairs in case of power outages, fires, and other emergencies. But if we substitute the major method of traversing floors in a facility to something safer than stairs, we can reduce the hazards that stairs pose. In the therapy world, this isn’t very functional because we know people use stairs at home and in the community. So let’s substitute actual flights of stairs with wooden framed in steps with handle bars on both sides. That will allow patients who need to perform stairs to practice them in a safe environment and reduce the hazard risk.
Engineering Controls. Ok, so let’s go back to the point of the hospital already being built and there are stairs. Can’t get rid of them. No problem. Engineering can come in and add controls. These types of things include hand rails, vertical bars on the turning platforms, gripper tape to the surfaces, yellow striped hazard tape to the edges of the steps, doors to the stairwell, and badge-locks to the doors. All of these things can help prevent the stairs from being as much of a hazard. There are many examples of engineering controls that apply to infection control, too, and we will investigate those later.
Administrative Controls. Policy policy policy. Change the policies, change the hazard risk. If it is policy that no one allows a patient on the stairs without supervision and assistance, odds decrease that the patient will get hurt. You can start to really see by now how these levels becomes less effective as we move down the pyramid.
PPE. For the sake of our stairs example, we are going to call a gait belt PPE. If we are going to use the stairs with someone who is unsafe and be there to provide them support, we can use equipment to decrease the risk of the training we are providing. However, placing the patient actually on the stairs for training is also the behavior that puts them at the highest risk of being injured. But we have to do it, right? So we use the gait belt to give ourselves a hand. It is our personal piece of equipment that helps (a bit) to prevent a hazard.
So how does all of this apply to viruses? Physical hazards are much easier to remove from the situation, but viruses can’t be fully removed. And substituting a different, less dangerous virus isn’t really a better option, nor is it feasible. So we have to come down to environmental controls next. Negative pressure isolation rooms are the most common thing we probably think of when it comes to treating patients who have a contagious condition. They are used for patients who have measles, influenza, and tuberculosis. The negative pressure room keeps all the air breathed in that room away from other rooms. The air is exchanged out individually, not entering the general air supply in the facility.
Speaking of the air supply, again, we are going to get a bit science-y here and talk about some fluid dynamics. Did you know that HVAC systems for hospitals actually have settings that allow for increased or decreased air exchange based on the square footage of the space and the concentration of people in it at any given time? Some can be self-altering based on occupancy, and some are static and have to be manually changed. A recent study was released that measured the air flow necessary to clear certain sized rooms with certain occupancy that would be required to reduce the transmission probability specific to COVID-19. They actually have it measured out how many cubic meters per minute of air they have to move so that no one would have to wait between using the bathroom for the air to be cleared (that’s 10 m3/min or 200 CFM (cubic feet per minute) for a single occupancy bathroom). For shared common spaces, the airflow needs to be 50 m3/min (or 2000 CFM) if the occupancy is fixed. If you are utilizing a public bathroom with several people in and out, the risk of transmission is difficult to control with this tool. Even air circulation patterns alter infection transmission which really comes in to play in oddly shaped spaces. If you are eating in a restaurant tucked away in that romantic corner, you are going to be more likely to transmit and/or receive transmission of infection due to lack of ventilation of aerosolized particles that are delivered to the space via “leaks” from the primary circulation of air in the restaurant.

While reading this article, I was thinking to myself, “So what is likely the highest risk thing or place right now based on these factors?” And the article didn’t disappoint. A choir practice in Seattle was studied as an epicenter of outbreak. The airflow in the small church was 20 m3/min and the choir had 60 members present for a 2.5 hour practice. The result of this practice was that 87% of the attendees became infected with COVID-19 from a single source. The authors discussed that choir practice significantly increased the rate of aerosolization with singing (this wasn’t the only choir outbreak) and that other activities such as indoor dance practices and working in a call center would be similar in transmission rate even IF hand hygiene and social distancing were utilized properly.
All of this to really demonstrate that Engineering controls can be put in place to prevent or decrease risk of transmission, but they have to be used properly. And if they are not, other measures put in place like hand washing and social distancing (both environmental controls as they try to remove the contagion) have little effect.
Why am I harping on about engineering controls? Why am I becoming concerned about the amount of air my HVAC system can move? This is why. New findings from this study include
- 1 min of loud speaking generates at least 1,000 virion-containing droplet nuclei that remain airborne for more than 8 min
- the smallest droplet nuclei effectively remain airborne indefinitely and have half-lives that are dominated by the ventilation rate, at a saliva viral load of 7 × 106 copies per milliliter
- Some patients have viral titers that exceed the average titer of Wölfel et al by more than two orders of magnitude thereby increasing the number of virions in the emitted droplets to well over 100,000 per minute of speaking.
- The droplet nuclei observed in this present study and in previous studies are sufficiently small to reach the lower respiratory tract, which is associated with an increased adverse disease outcome
In essence, talking is sufficient to aerosolize COVID-19 particles and these particles remain in the air for at least 8 minutes. Then pair that with this study with these findings:
- airborne transmission, particularly via nascent aerosols from human atomization, is highly virulent and represents the dominant route for the transmission of this disease [COVID-19]
- the importance of airborne transmission has not been considered in establishment of mitigation measures by government authorities
- And my personal favorite: It is also important to emphasize that sound science should be effectively communicated to policy makers and should constitute the prime foundation in decision-making amid this pandemic.
All three of these studies referenced recommend personal use of face coverings/masks as the only way to effectively reduce viral transmission and their effectiveness if increased with the addition of other controls such as social distancing and hand hygiene. However, these other controls are not effective without the use of face coverings/masks. For how to make a homemade mask that might actually work, check out this post.
So even though PPE is literally the WORST at controlling infectious transmission, and even though it truly is the last line of defense against transmission, it will end up being the best bet we’ve got. We can’t always control the environment we are in. We can’t substitute a different pathogen that is less virulent. We can implement engineering controls in the facilities we utilize, but not in the community or outdoors. We can add administrative controls to reduce the risk of infections. But ultimately, with COVID-19 and other respiratory pathogens like Measles and Tuberculosis, it’s going to come down to the PPE. Especially in the rehab professions, where close contact and use of different speech techniques are regularly utilized across disciplines, we need to be taking precautions, educating ourselves, and keep each other safe.
Do you work in environmental infection control? How has COVID-19 changed your day-to-day? Tell me in the comments!
Follow my blog for more!
References
Evans, M. (2020). Avoiding COVID-19: Aerosol guidelines. Massachusetts Institute of Technology: Department of Physics. Published by medRxiv [ahead of print]. Retrieved from https://doi.org/10.1101/2020/05/21/20108894
NIOSH. (2015). Hierarchy of Controls. Retrieved from https://www.cdc.gov/niosh/topics/hierarchy/default.html
Stadnytskyi, V., Bax, C. E., Bax, A., Anfinrud P. (2020). The airborne lifetime of small speech droplets and their potential importance in SARS-CoV-2 transmission. Proceedings of the National Academy of Sciences. 117 (22) 11875-11877; DOI: 10.1073/pnas.2006874117
Zhang, R., Li, Y., Zhang, A. L., Wang, Y., Molina, M. J. (2020). Identifying airborne transmission as the dominant route for the spread of COVID-19. Proceedings of the National Academy of Sciences. 202009637; DOI: 10.1073/pnas.2009637117

Follow @DoctorBthePT on Twitter for regular updates!





Like!! Really appreciate you sharing this blog post.Really thank you! Keep writing.
LikeLike