It may be in short supply, but that doesn’t mean we don’t need it. Any therapist performing respiratory techniques (the ones COVID patients probably need!) is at risk and should have the right PPE. Here is what you need, what you can get by with, and how to choose.

The Mask
We are all hearing the hysteria around the mask right now. Surgical vs. respirator vs home made. How and when do you choose what?
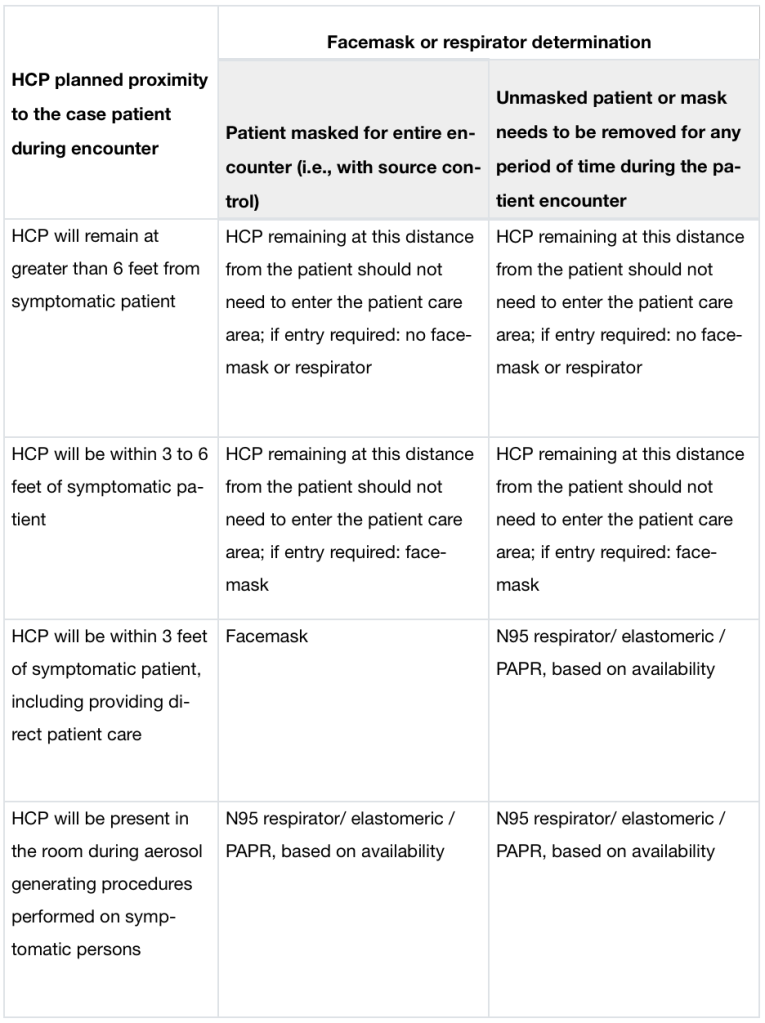
The CDC has created a table with some guidelines on how to make these choices. It’s important to remember where Physical Therapists fit on this table. If you are performing respiratory physical therapy interventions, you are performing aerosol-generating procedures (AGPs).

Gloves
Thankfully we aren’t hearing too much about a shortage of these yet! You should just be wearing them. Odds are you know this already. Both hands, please. And make sure your friends wear them, too. You can reuse if necessary by using gel hand sanitizer with at least 60% alcohol to clean them between patients. If gloves are visibly soilerd they must be changed.

Gowns
So stylish. So crinkly. One use, one patient. Do you remember the order in which you are supposed to don all this stuff? Yea, I didn’t either. Here’s a link to help you out.

Eye Protection
We are still under droplet precautions. However, most sources disagree with this and feel we should be under airborne precautions. Either way, you’ll need some eye protection. Goggles or a shield are acceptable. There are also eyewear choices available on Amazon that seal around the eyes and may be approved by your individual facilities.
all images open source from upslash.com
Check out these other links:
A homemade mask that may actually work?
Maybe! Check it out!
Forbes is putting the word out. Like the doctor said: “Any mask is better than no mask.”
Calling All People Who Sew And Make: You Can Help Make Masks For 2020 Healthcare Worker PPE Shortage
Home (Health) is Where the Heart Is
Dr. Rebekah Griffith, other wise known as The ED PT, interviewed Dr. B on all things patient care management and how PTs in the ED and Home Health PTs can work together to provide the best possible care for patients. We talked about the struggles we each face in managing complex patients and the roles…
Expanding Your Role, Fulfilling Your Scope
BONUS CONTENT! How can you build primary diabetic care (and other chronic disease care) into your PT practice? Take a read here!
Primary Care PT
PTs primarily treating diabetes shouldn’t be a far cry from the future, it should be today! Read this for more!

Follow @DoctorBthePT on Twitter for regular updates!