During her address to the House of Delegates this year, President Dunn quoted Mary McMillan‘s statements as she traveled back through the history of our profession…
“A physical therapist should keep up with the latest in her profession so that when new things come along she is aware of them, so that she may be of greatest service to her patients. She must believe in herself, for without this, others cannot have faith in her. She must have faith in herself, and that does not mean cocksureness, that all too frequently comes from ignorance. A physical therapist must never let her patients go without hope, and I do not mean false hope either, I mean real hope. Because hope helps to chase away fears. Of course, it’s not always easy. There will be hard knocks. It is the hard knocks that help to bring out the best timber in us. Who wants a soft job, anyway?”
Mary McMillan
Many of you know that I used to work in home health for several years. It was during my time in home health care that I learned the meaning of practicing to the fullest extent of my license. This is my second soap box (vitals are vital being the first), and I want to step up on to it for a minute.
If you’ve worked in home health, you know all too well how this goes. You admit the patient under the hospitalist or the primary care or whatever random doctor the patient names for you. You call them with your plan of care (Yes, this is what home care is required to do. No, it can’t just be in writing.) and they say something along the lines of, “I haven’t seen the patient in 3 years! I’m not signing for this,” or “I’m just the hospitalist/rehab doctor, I’m not signing for home care.” So now you are left to figure this out and hope your medical director will sign for services until the patient can be seen by someone for their face to face visit (another home care requirement). This means you are the only care provider managing this case. This means you are providing primary care in the home setting to some of the sickest patients.
COVID-19 has changed the way we practice. And if you don’t think so, you shouldn’t be practicing. PTs have had to step up and show what we are made of, what we can do, and how much we actually know. All I have to say is: It’s about time!

More often than not, when patients return home from a subacute setting to the home setting, they are returning home with one or no caregivers. They may even be returning home with one or no other providers involved in their care (see example above). As physical therapists, practicing to the full scope of our education and license is going to be all the more important. We are now the front line against community spread of COVID-19. This doesn’t just apply to home health, but also to outpatient services. We are also the front line to prevent further health decline and hospital readmission. We are the front line to manage medication and assess health status. We are the front line to differentially diagnose whatever other impairments and conditions may be present. We are the front line to request assessment, tests, and other items that may assist us in patient care. We are the front line in screening for other health factors such as social determinants of health, safety in the home, and hidden health impairments.
So what does that mean for our practice? It means that your job now includes things that it may not have included. For some time, in the home setting, we were screening all patients for Zika, Ebola, and SARS. COVID-19 screening is now going to be common place for every new patient. It is also going to be common place for every patient visit. If you can’t get your nails done without getting your temperature taken, you definitely shouldn’t be in a physical therapy clinic without it. And while you are taking your patient’s temperature (or your aide is), why not also take their heart rate and blood pressure? Let’s screen for hypertension, too. Maybe even catch some early heart failure? That’s what providers do. If you walked in to see a primary care doctor and didn’t have your blood pressure taken, would you even bother going back? I wouldn’t. In the outpatient world, we are providing primary care, so let’s act like it.
It is now our primary job to ensure these patients are receiving screening for the cognitive and mental health effects of their COVID-19 experience and for the cardiovascular impairments they may be experiencing beyond the generalized weakness and difficulty with ADL. We have talked in previous posts about the side effects of ARDS, PICS, mechanical ventilation, ECMO, proning, and so many other interventions these patients may have experienced. The side effects amount and most of them are within our scope of practice to screen, evaluate, and treat. Anxiety and depression already have a bearing on participation in exercise as well as the pain experience, so when is the last time you screened for either? When is the last time you applied exercise as the treatment of either? There is plenty of evidence to back it up.

We know that the risk for clotting increases significantly (Read more here!) so screening for DVTs and PEs may become something done at every visit. That also means screening and considering the increased risk for strokes. We also need to be establishing a baseline for delirium and other cognitive factors that can change as a result of COVID-19 like we discussed here. Set the baseline and document improvement through skilled assessment over time!
Sure, sure. Taking vitals is not a skilled or billable service. But your interpretation of vitals IS a skilled procedure. This is how you determine your patient’s safety to participate in exercise, or if they might have a PE, or if they are clinically hypertension. I promise you, we are not looking for zebras amongst the horses. We are just looking at the horses. And if you don’t look, you won’t see them until they are stampeding over you.
Beyond screening, we also need to provide interventions for these impairments to the fullest of our abilities. If this care is outside of our scope, we need to be making the referrals necessary to ensure these patients receive the proper interventions from the proper providers within our interdisciplinary team. Education is a huge part of our skillset. I often say that, as instructors in PT programs, we are not just teaching physical therapists, we are educating educators. Education on any of these topics, as well as lifestyle modification interventions, are going to start taking their place front and center in our profession, so be ready.
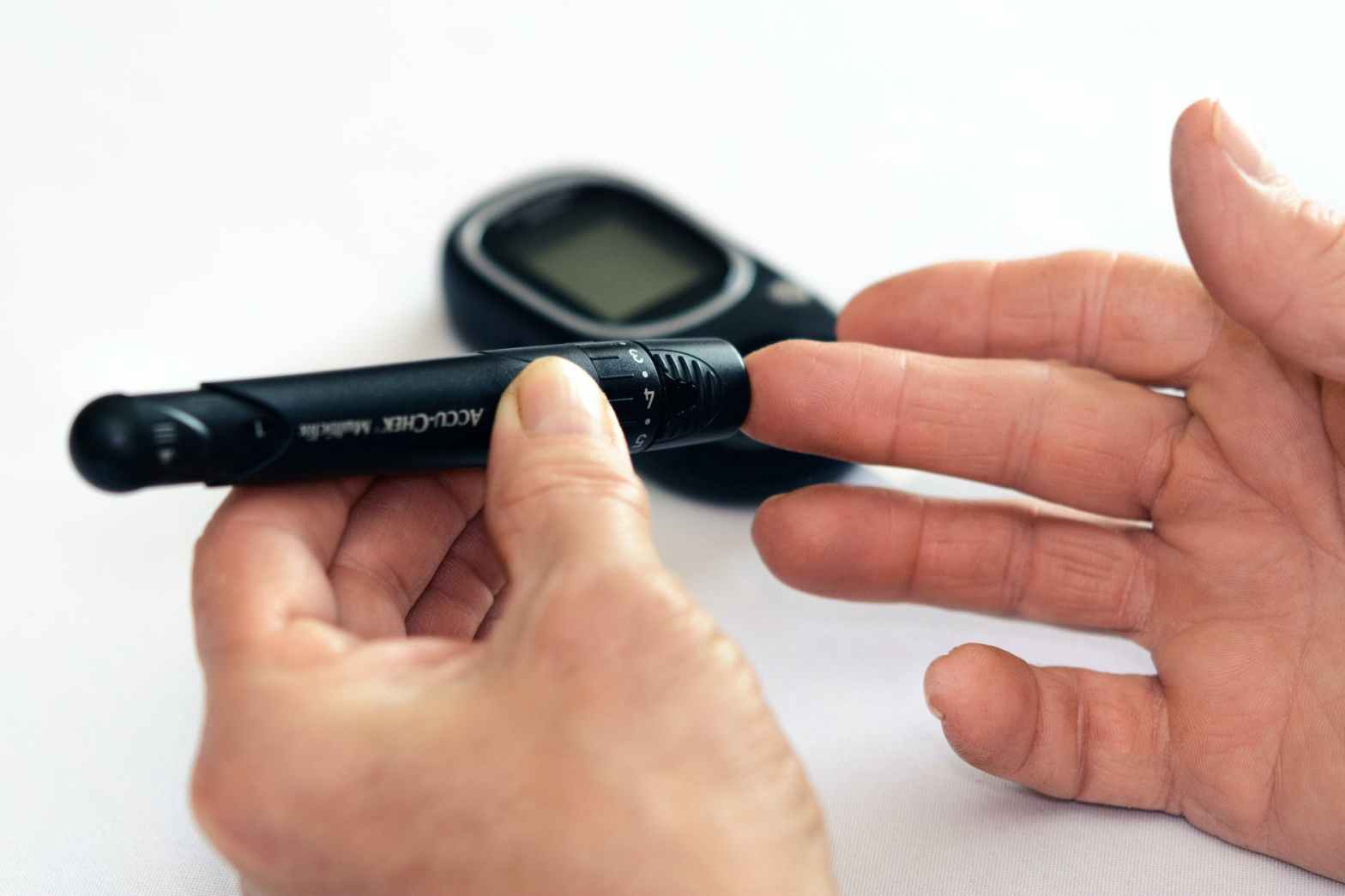
For some of us, this may not be new. Some of us may have been doing this for some time. Medicare deems physical therapists competent to provide services like medication reconciliation and management, anticoagulation monitoring (PT/INRs) (yes, we do minor blood work), and perform diabetic teaching including the use of blood glucose assessing devices. We need to consider the ability to request labs: UAs to check for urinary tract infections, CBCs to check hemoglobin status, dopplers to check for DVTs, plain film radiographs after a fall, and ABGs when concerned about advanced COPD and oxygen use. (Of course, you better have some good reasons to back up your requests and a good relationship with the physician helps!) If you think about it, all of these things are necessary for us to provide whole-patient care and ensure our patients are safe to perform exercise. Even if Medicare didn’t deem us competent, we were educated to be.
Don’t know how to do this or where to start? Head on over to SRA Lab and take a looksee at their RehabMeasures database. Some of you may remember this as “rehabmeasures.com” but that doesn’t exist anymore. The new site is packed full of screenings and tools that are validated for PT use in any patient population you can think of and for almost any diagnosis. Bonus: most of them are free!
- Need an assessment of caregiver strain for your patient who has cancer? They’ve got that.
- Suspect depression your geriatric patient with COPD and diabetes? They’ve got that.
- Forgot how to quantify tone for your patient who had a stroke after COVID-19? They’ve got that.
President Dunn’s address reminded me of some of the topics in my Podcast with my home health friend Afrin where we looked back in history at how PTs have responded to pandemics and other crises. This is what primary care management looks like. This is the role we need to take on and it’s the role we were educated to fill. Who wants a soft job, anyway?
How do you provide primary care? Tell me more in the comments!
Follow my blog for more!
If you want to watch all of President Sharon Dunn’s address, check out the link!
References
Mayer, K., Engel, H., Falvey, J., Ricard, P. (2020). COVID-19: ICU to Home Transitions. [Webinar] Home Health Section of the American Physical Therapy Association. Retrieved from https://aptahhs.memberclicks.net/assets/5-16-20%20ICU%20Webinar%20Recording.pdf

Follow @DoctorBthePT on Twitter for regular updates!




13 thoughts on “Primary Care PT”