Let’s start with a story…
Man on a Train
I was exiting a train on the platform at Reagan Airport when suddenly I see a man falling back onto the train as it was pulling away. His eyes were rolled back and he looked limp. My husband and I pulled him off the moving train that was starting to carry him down the platform. He was somewhat conscious, enough to get a faint mumbled medical history which included diabetes. He swore he had eaten this morning, just an apple, but he knew his blood sugar was fine. I checked him for injuries and monitored him until first responders arrived.
I passed on the history of diabetes to the first responders. Their first task was to take his blood glucose. It was in the 30s. His apple had not been enough or there had been some issue with his medications and he was tanking fast. I had some candy, so we gave him that, and they took him away in the ambulance.

I feel like Physical Therapists should be on the front line providing treatment for diabetes. Yes, I said front line, and yes, I said treatment (and I’m not alone in that!). And not just because up to 80% of the patients referred to us HAVE some type of diabetes! But, we have definitely not positioned ourselves this way. We currently treat diabetes as a comorbidity, when really it’s almost always the primary concern.
Diabetic with a broken leg? Diabetic changes to the blood vessels resulted in poor nutrient circulation to bone tissue resulting in decreased bone quality.
Diabetic with cancer? Systemic declines in immune function secondary to diabetic changes reduced the ability to fend off cancer.
Diabetic with a wound (even a surgical wound)? Healing is going to take twice as long, if not more because diabetic changes to the tissues and vessels will reduce the ability to heal. Diabetes may have even caused the wound to start with!
Diabetic with a frozen shoulder? Don’t even get me started…
So, why don’t Physical Therapists position themselves to treat diabetes? Well, it’s pretty hard to make exercise sound like a better treatment than taking a single Metformin every day… But, I’m here to give it my darndest.
Managing Type 2 Diabetes
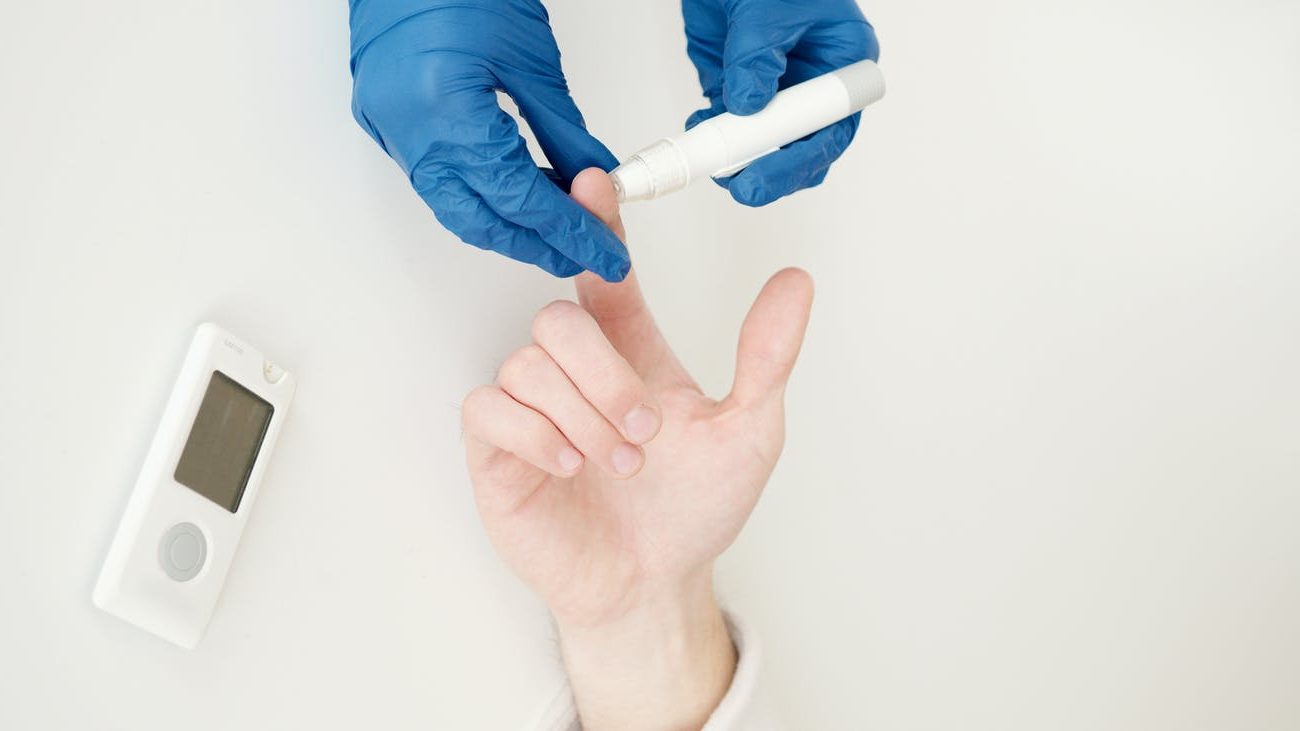
Blood glucose monitoring. Your ability to do this may vary based on your state, but we all know the importance of blood glucose levels for exercise. If we don’t time our sessions properly, we end up with a patient passing out on us. If we do time them properly, we can actually (over time) decrease or eliminate the need for medication to manage blood glucose. Let’s talk about the logistics of this:
- To clear up the risk analysis: If your patient is already diabetic, they already have a physician’s order to check their blood glucose daily. If you ask them to or assist them in doing this prior to your session or during your session, you are in full compliance with this order. If you need to do this for your patient because they are unable, you are still in full compliance with this order. If your patient’s blood glucose is so low that they are unable to measure their own blood glucose, are you going to sit there wondering if it’s ok while they fade away? No, of course not. You should probably be calling 911 at that point, but take their blood glucose. (Side note: please wear gloves.) Diabetic teaching is well within our scope of practice. So is diabetic intervention (aka exercise). PTs can even become certified diabetic educators.
- You cannot administer insulin if your patient’s blood glucose is too high unless you are trained to use the devices to do so and there is an order in place (if your patient is diabetic, there is an order in place, but you have to know how much, i.e. sliding scales and all that). You should be calling the physician or nurse case manager for instruction if your patient cannot self-administer. You can, on the opposite end of the spectrum, give your patient food. You should have fast-acting sugars available in your clinic: juice, candy, applesauce… Even in outpatient clinics, I’ve given juice when I noticed the signs of hypoglycemia.
- You, yes YOU, a rehab clinician, can educate patients on diet, how to use a glucometer, and how to use a sliding scale. It is within the scope of practice of a physical therapist to educate on medications as the primary case manager under Medicare guidelines. If you can do an OASIS, you can teach meds. As a matter of fact, it is EXPECTED that you complete the meds teaching to the best of your ability and consult nursing for the rest. Sliding scales are provided for you by the primary care physician or endocrinologist, so you just explain how to use them. If you aren’t sure, check out some online training courses to get more information.
Not My Patient
I made a home visit to evaluate a very kind woman who did not want my help. She wasn’t rude, she was just straightforward. As her doctor did order PT for falls, I talked her into letting me do a walk around the house with her.
It wasn’t her house, she told me. She was just staying with family for a while until she felt better. We walked through a few rooms and saw a few different people. It wasn’t their house either, she explained. Her family takes in people who need some help until they can get back home. She was walking fine without a device, albeit a bit slow over the changing carpets in this piece-meal home.
We passed by a bedroom where her sister-in-law was shaking a man lying in bed. The woman was audibly yelling at the man who was only somewhat mumbling back to her. I sat back down at the dining table with my patient who clearly told me she was fine. And then I hear the words from the other room…
“530? What does that mean? What’s his sugar supposed to be?”
I smiled at my patient and said, “if you don’t want me to come to see you, that’s fine with me. That man right there is in trouble. Would you mind if I helped him?” She smiled and said, “of course, honey, he’s been real sick.”
I ran to the room and did a recheck on the glucose. The 530 was just the most recent on the glucometer history. The actual was 615. He was losing consciousness when I called 911. The family gave me a first name and age but I had no other medical information. The paramedics were quick to arrive and stretchered him quickly to the ambulance.

What ARE the signs of hypoglycemia?
I’m so glad you asked!
- Arrhythmia
- Fatigue
- Palor
- Sweating
- Anxiety/mood changes
- Confusion
- Lightheadedness/headache
- Shaking
- Unsteadiness
- Anxiety
And one list is not complete without the other…
What are the signs of hyperglycemia?
- Fatigue
- Weakness
- Confusion
- Nausea/vomiting
- Shortness of breath
- Dry mouth/fruity breath
- Urinary frequency
- Headache
- Blurry vision
Now look at those two lists… lots of similarities there… so it may be difficult to actually tell if your patient is hyper or hypoglycemic. This is why you will need to check their blood glucose.

The Need to Know
Just like with pulse oximetry for patients with respiratory conditions, blood glucose in people with diabetes is something I NEED to know. I need to know what it is before exercise, what the trends are, and what it is first thing in the morning. That’s how I know if the diabetes is well-managed or not and determines how and when I prescribe exercise.
What are safe parameters for blood glucose?
I thought you’d never ask! Here’s the meat and potatoes. Let’s put these numbers in order from least to most and make a scale. Remember, these numbers assume the person already has a diagnosis of type 2 diabetes.
Too Low
<50 mg/dL
call physician/911 based on symptoms,
give sugar
Too Low for Exercise
<70 mg/dL,
give sugar
Ideal Range for Exercise
100 – 250mg/dL
Too High for Exercise
>250 mg/dL call physician, risk of ketoacidosis
Too High
>350 mg/dL call physician/911 based on symptoms
If a patient with diabetes is participating in an exercise class or performing exercise in long bouts (longer than 60 minutes) blood glucose should be checked every 30 minutes to ensure ongoing safety to reduce the risk of ketoacidosis or hypoglycemia. Ketoacidosis is when there are too many ketones in the body. For diabetic people, this can be life-threatening. But, that’s a whole other condition, so we will talk about that later. Just know that it is a medical emergency and refer to my friend above who wasn’t my patient.
Effects of exercise (which are many!) on blood glucose only last 24 hours, so some type of exercise should be performed EVERY day for long-term stabilization and management. And, as I usually make the statements about properly prescribed exercise, that all applies here, too. Set a baseline exercise tolerance or aerobic capacity, measure vitals, calculate heart rates, and exercise to the proper ranges. Not only will this help manage blood-glucose long-term, but it will help reduce pain associated with peripheral vascular changes due to diabetes, too.
Don’t Forget Diet
Nutritional counseling is well within our scope of practice as rehab providers, especially if our patients are diabetic. It isn’t even safe for our patients to exercise without knowing the basics of how energy input and energy output affect their health status.

Don’t be shocked if your patient doesn’t know where sugar comes from, what carbs are, or if bread is a protein or not (very serious, I had that exact conversation once). Some people take it upon themselves to know a lot about their health and what they can do to manage it, but many people don’t. Their health is something that happens to them, not something they actively participate in. So, it will take a lot of counseling to get their energy inputs and outputs back on track.
Don’t forget to call on your handy dandy dietician, too. Diabetes takes a team. Hopefully, you are on that team and can help the patient balance those energy inputs and outputs and keep them safe while you do it.
Keep in mind that the more comorbidities your patient has, the harder it will be to control their diabetes. Many medications and other conditions impact blood glucose and just throw the whole thing off! Goodness, so much to cover and we haven’t even gotten to the feet yet! I guess the diabetic foot will have to be another post. Keep checking back for Part 2 and I’ll keep your brain busy! I’m definitely not done yet!
How often do you teach patients how to use their glucometer? Tell me about it in the comments!
Get new content delivered directly to your inbox.
More Reads…

Follow @DoctorBthePT on Twitter for regular updates!
References:
Liu, Jx., Zhu, L., Li, Pj. et al. Effectiveness of high-intensity interval training on glycemic control and cardiorespiratory fitness in patients with type 2 diabetes: a systematic review and meta-analysis. Aging Clin Exp Res 31, 575–593 (2019). https://doi.org/10.1007/s40520-018-1012-z
Magalhães, J.P., Melo, X., Correia, I.R. et al. Effects of combined training with different intensities on vascular health in patients with type 2 diabetes: a 1-year randomized controlled trial. Cardiovasc Diabetol 18, 34 (2019). https://doi.org/10.1186/s12933-019-0840-2
Marcie Harris-Hayes, Mario Schootman, Jeffrey C. Schootman, and Mary K. Hastings. The Role of Physical Therapists in Fighting the Type 2 Diabetes Epidemic. Journal of Orthopaedic & Sports Physical Therapy 2020 50:1, 5-16
Mayo Clinic. (2020, May 13). Hypoglycemia. https://www.mayoclinic.org/diseases-conditions/hypoglycemia/symptoms-causes/syc-20373685
Mayo Clinic. (2020, June 27). Hyperglycemia. https://www.mayoclinic.org/diseases-conditions/hyperglycemia/symptoms-causes/syc-20373631
Centers for Disease Control and Preventions. (2021, April 28). Diabetes: Manage Blood Sugar. https://www.cdc.gov/diabetes/managing/manage-blood-sugar.html
The contents of this blog and all associated pages reflect the opinions of the author and should not be construed as medical advice. Please consult your doctor for medical advice.








One thought on “Chronic Disease Part 4: Type 2 Diabetes – Part 1”