If you are going to be providing pulmonary interventions, you should probably have a strong idea of how to auscultate the lungs. The importance of this is pretty paramount. You have to know WHAT you are listening for and you have to know HOW to listen. There are a lot of variables when it comes to disease state, but if you have a stethoscope, just start listening to all your family members to get an idea of what “normal” sounds like.
The method of performing auscultation that gives you the most information is to use the “S” pattern. This includes listening from top to bottom and left to right with the ability to compare right and left sides of the same lung segment. You also MUST listen to both the front and back of the lungs to ensure you are getting all the segments. If you don’t, you may miss the left lingular segments which is where stuff likes to hide.
So let’s start with the basic anatomy refresher. We aren’t going to spent too much time here. What is most important is that you listen to all segments and compare sides.

When auscultating, you want to start in the same place every time, typically the patient’s right upper lobe, then traveling across the sternum to the left upper lobe, then inferiorly, and then across. This is what creates the “S” pattern.

Moving On…
The How To:
Listen at each point for two full breaths. Keep in mind that WHAT you hear depends on what depth of breath is being taken. Shallow breaths don’t move air in the bases of the lungs so you don’t typically hear sounds there! However, hearing NOTHING is also a problem! If you don’t hear anything, here’s what to do:
- Check your stethoscope! Some have heads that swivel to channel sound toward different sides (bell vs. diaphragm). If the head got turned, you won’t hear anything.
- Look down. This helps reposition the ear pieces to channel the sound directly in to your ears. You can also lift the ear pieces upward, same effect.
- Ask your patient to take a deeper breath.
- Listen longer. A typical respiratory rate is 12-16 breaths per minute. This is one breath about every 4 seconds. If your patient is bradypnic, you may have to wait longer.
What Should You Hear?
Normal lung sounds (named “vesicular” sounds when auscultated over the peripheral segments) should be somewhat quiet, but sounds that are too quiet are what we term “diminished.” It can be typical to hear diminished sounds in a patient who is obese or who doesn’t utilize much lung volume. If they are not utilizing much lung volume, this is a great opportunity for you to intervene with some diaphragmatic breath training and/or IMT use for diaphragm strengthening!
Other normal sounds include bronchial (which are only normal when auscultated over the bronchials) and bronchovesicular (which are only normal when auscultated over the bronchioles).
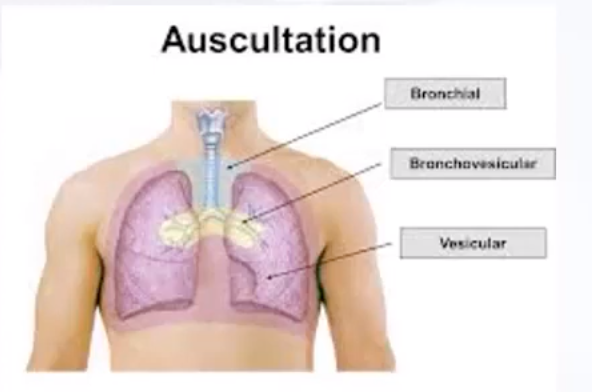
It is important to remember that a normal sound that is auscultated in a place not considered to be normal is an adventitious sound.
Adventitious Sounds
An advantage for you, not for your patient… Adventitious sounds can be used to determine what pathology is present and what treatment needs to be performed.
Crackles (also known as “Discontinuous sounds”) can be heard over the peripheral airways also. Crackles can be a sign of COPD, bronchitis, CHF, Pneumonia, or atelectasis depending on when they happen in the breath cycle. Crackles can be fine (like bubbles gently popping) or course (like tearing Velcro apart). These sounds should tell you that you need to perform some interventions. ACBT helps with this.
Stridor is going to be a very important sound to know when assessing or treating patients with COVID-19. Stridor is typically associated with upper airway narrowing. However, it may also be present in extubated patients who come home after being hospitalized. If stridor is just beginning, your patient may need some urgent medical intervention. Hopefully, they will be moving toward the end of it.
Rhonchi (also known as “low pitched continuous sounds”) are what I’ve always termed “the goose honk”. Rhonchi are heard when large amounts of mucus are present in the larger airways. These types of sounds are good indicators that some pulmonary hygiene is needed. ACBT is really useful here, as well as FETs or a PEP if your patient is too weak to perform FETs well. And sometimes you just need a good cough. If this patient has a trach, they will need suction.
Wheezes (also known as “high pitched continuous sounds”) are a fairly common adventitious sound that many people have heard. There are several tones and types, but overall, they indicate airway obstruction of some degree. You need to intervene here with some pulmonary hygiene interventions. ACBT is particularly useful here because wheezes can be in the smaller airways which can be targeted with ACBT. Segmental breathing may also be helpful if you can pinpoint the segment through your auscultation. PEP may also be useful.
Absent lung sounds can mean serious issues. If you have already tried the above techniques to modify what you hear and have had no luck, and your patient appears to be struggling, they may be experiencing a pneumothorax or severe atelectasis and you are auscultating right over it. There could also be something other than lung tissues present. If there is a tumor or other object that does not perform gas exchange in that particular location, you won’t hear air movement.
Please also check your patient’s medical history. If you are experiencing absent sounds, your patient may have had a lobectomy and there is no lung tissue present where you are auscultating.
If you happen to hear gargling sounds, you are auscultating too far inferiorly and have hit a digestive organ!
I also auscultate AFTER performing interventions and like to document the secretion movement (because you may hear it somewhere else after interventions) or the lack of adventitious sounds along with improved patient presentation indicating that secretions are no longer impairing ventilation!
BONUS!!! I found this video specific to adventitious sounds present in patients with COVID-19. You’ll hear the combination of several of the sounds you just listened to!
Now get to listening! Remember, you have to know what normal sounds like, so make sure you are listening to as many lungs as you can!
Comment below to tell me about a crazy sound you’ve heard while performing lung auscultation!

Follow @DoctorBthePT on Twitter for regular updates!





11 thoughts on “The Basics of Lung Auscultation”