I took a trip to Denver recently and, right around the same time, was consulted regarding the use of a pulse oximeter at high altitudes. It all got me thinking: how different could it really be to practice at 9,000ft? So, I did some work on this and I have to tell you, finding this information was nowhere as easy as I thought it’d be. Apparently there is a very specialized branch of medicine known as “mountain medicine” or “altitude medicine” that is the established group of experts on the changes altitude can have on human physiology. The primary article I’m referring to for this post was written by Luks and Swensen, the same two who wrote the guidelines on using pulse oximetry for monitoring COVID patients for the American Thoracic Society. I’m excited to tell you all about what I’ve learned!
First off, we all know that as we go higher, there is less usable oxygen in the air. That is, the fraction of inspired oxygen (FiO2) remains about the same at 20.9% but the pressure of the oxygen (PiO2) decreases. Anyone remember Boyle’s law from junior high? That’s what we are talking about here: the inverse relationship between pressure and volume. Essentially, increased pressure results in decreased volume and, therefore, increased concentration of a given component. The volume of air we have under our atmosphere doesn’t change (the space stays the same), but as we ascend to higher altitudes, the pressure of gravity lessens, so the concentration of oxygen also lessens.
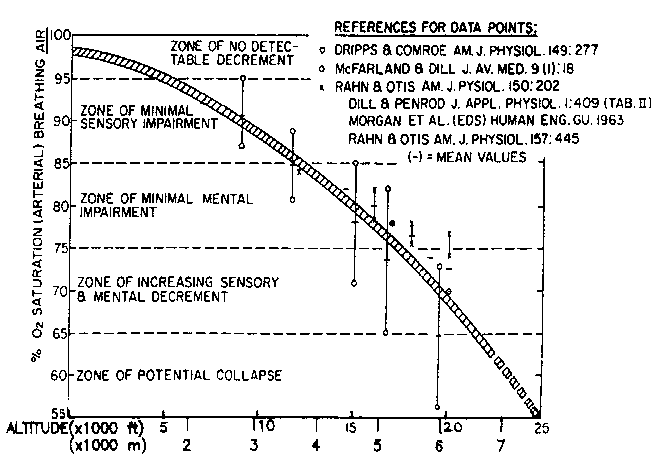
You may have heard this referred to as “thinner air” which is far more accurate than saying there is less oxygen. This change influences our body’s ability to diffuse the oxygen into our lungs and perfuse it into our tissues, impacts the oxygen-hemoglobin dissociation curve, and begins the process of significant physiological change. This graphic gives a percent of oxygen pressure at varying altitudes.
Based on this table, you may think that patients (or people in general) would become breathless pretty easily around 5280 ft (1 mile), but that’s not the case. Most people don’t feel any effects of altitude in regular daily activity until at least 4000ft, with the greatest majority of people experiencing effects around 7500ft. Of course, because our patients tend to be patients for a reason (they are more sick than the average person), they may start experiencing effects somewhat below those elevations.
At VERY high altitudes (above 11,500ft) the maximum amount of oxygen your blood can carry decreases to about 90% or less (your maximum blood oxygen saturation – SaO2 – is 90%), which will then result in significant breathlessness with activity. And above 20,000ft, we don’t expect to see long term human habitats due to severe physiological impairment. The presence of cardiovascular or pulmonary disease will result in symptom onset at lower altitudes than expected.
Training and Rehabilitation At High Elevations
The biggest challenge in practicing at higher elevations comes with seeing patients who are not regular residents in these areas. If your patient has been in the mountains for two weeks, their body has had time to accommodate. They will produce more red blood cells, hemoglobin molecules, and become more efficient at perfusing tissues (their oxygen-hemoglobin dissociation curve shifts to the right). This may take a bit longer if your patient has underlying medical conditions. Some people actually use this physiological adaptation to their advantage. Let’s look at that.
You may have heard of blood doping? That is where people (usually athletes) go to higher elevations to train for their sport because the altitude will cause them to develop this hemoglobin-rich blood that is so much more efficient at carrying oxygen, especially when they go back down to a lower elevation, which results in better aerobic performance. Although clever and a fully drug-free way to enhance performance, (which can also be achieved through transfusions, drugs that modify the oxygen-hemoglobin dissociation curve, and erythropoietin injections) the practice was outlawed in professional sports in 1986. This was due to a huge scandal at the 1980 Olympics that resulted in 17 medals being relinquished because of blood doping. However, if you are just looking to enhance your own sport performance outside the roles of professional sports, head up to 6,000ft!
When prescribing and performing activity at higher elevations, you should see a fairly quick rebound in healthy people once they start to rest (less than 5 minutes). However, you’ll eventually run in to trouble because even healthy people don’t have enough Hemoglobin to carry O2 for longer bouts of activity if they aren’t accommodated to the altitude. You may have to use shorter bouts and regulate the intensities to maximize oxygen supply (high-intensity interval training would be great for this!).
So how does altitude impact pulse oximetry?
Thankfully, it doesn’t, at least not significantly. As you move toward higher elevations, the “normal” O2 saturation as measured via a pulse oximeter just becomes a bigger range due to a larger standard deviation in the tool. And, the lower the saturation measurement (like in a symptomatic patient), the larger the standard deviation in the readings. Around 4000ft, the first standard deviation found in pulse oximetry readings encompasses a range of 5-7% difference when compared to SaO2 (the oxygen saturation of arterial blood – not the same thing as SpO2). You also may find more symptoms in patients on Sulfonomide antibiotics (Bactrim, Augmentin, etc) as these drugs shift the oxygen-hemoglobin dissociation curve and can cause a decrease in useful hemoglobin. As we discussed HERE, this wont show up on your pulse oximeter but will show in the patient’s symptoms. The best thing you can do is make sure you are optimizing your use of the pulse oximeter by following the tips I provide HERE. Basically, you need to keep in mind that the more desaturated your patient becomes, the less you can trust your pulse oximeter to give you accurate readings.
Pulse oximetry should not be any different if your patients are residents or have lived in these elevations for a long time. If they are travelers, you may have a problem because they haven’t acclimatized. In this case, you will definitely see a drop in pulse oximetry readings with activity because these people will burn up their smaller supply of oxygen pretty quick and they can’t pull enough oxygen from the air to replace the deficit. This is a problem with V/Q matching.
Is this what causes altitude sickness?
Odds of experiencing altitude sickness increase as your elevation increases, but typically doesn’t occur until 7500ft in healthy people. Some sources estimate between 20-40% of people who travel to this altitude will experience symptoms. Your fitness and activity level has no impact on whether or not you experience altitude sickness. What does matter is how quickly you ascended to the destination altitude!
Altitude sickness results from the body having difficulty responding to the lower partial pressure of oxygen in the air. Oxygen diffuses into the lungs based on a gradient from areas of higher pressure (the atmosphere at 760 mmHg) to areas of lower pressure (our lungs at 756 mmHg). That’s only a 4 mmHg difference in pressure that drives inspiration. Therefore, small changes in the partial pressure of oxygen in air can significantly impact this pressure gradient. As the pressure of air decreases to become closer to the pressure in our lungs, the gradient that drives inspiration becomes smaller and breathing becomes more effortful. We can actually predict the symptom onset based on altitude as seen in this graphic form the Mountain Medicine Association.
When we aren’t able to consciously alter our breathing to adjust to this, like when we are sleeping, our body experiences the effects of this pressure change which can make some people sick. Symptoms will usually occur within the first three days of arrival to a higher elevation, and as quickly as 6 hours after arrival. Symptoms of altitude sickness include:
- Headache
- Fatigue
- Lightheadedness or dizziness
- Lack of appetite
- Difficulty staying asleep (waking frequently)
- Nausea, sometimes with vomiting
Altitude sickness is common and not an emergency unless it does not stop after the initial three days. In our travel party to Denver of six adults and two children, one child experienced altitude sickness but made a quick recovery. That’s right, children are also susceptible, especially if they have underlying medical conditions. The Mountain Medicine Association provides extensive guidance for traveling to altitudes with children, as well as instructions on how to assess if a child has altitude sickness. The scale seen here is often used for vocal children. Our party member had a score of 7 on this scale. It is important to note that all symptoms must be present in the experience of a significant change in altitude.

Ongoing symptoms can lead to dehydration from the vomiting, but also because our body loses more water vapor through breathing at higher elevations. The most critical progression of symptoms can lead to cerebral edema with symptoms of confusion and significant lethargy (a condition know as High Altitude Cerebral Edema – HACE) or pulmonary edema with symptoms of tachycardia, shortness of breath at rest, and a nonproductive cough (a condition known as High Altitude Pulmonary Edema – HAPE). These two progressions can also afflict an acclimatized mountain-dweller who descend rapidly to lower altitudes. These more serious form of altitude sickness are less likely to occur below 7500ft, and the overall incidence even in expeditioners is less than 4%. However, they are life-threatening and require emergency medical intervention.
Avoiding Altitude Sickness
The only real way to completely avoid altitude sickness when traveling to higher altitudes is to ascend and descend slowly, and spend about a day in each 1000ft ascent after 3000ft before ascending further. People considered “low-landers” (aka those of us who live below 3000ft) and have a range of specific health conditions, should take caution when traveling to higher altitudes, or not travel to them at all. The Mountain Medicine Association provides this list for guidance:
Caution with travel to high altitudes:
Moderate chronic obstructive pulmonary disease (COPD)
Compensated congestive heart failure (CHF)
Sleep apnea syndromes
Troublesome arrhythmias
Stable angina/coronary artery disease
Pregnancy
Sickle cell trait
Cerebrovascular diseases
Any cause for restricted pulmonary circulation
Seizure disorder (not on medication)
Young children
Avoid high altitude:
Sickle cell anemia (with history of crises)
Severe COPD
Pulmonary hypertension
Uncompensated CHF

However, we know very well that Physical Therapists and other Rehabilitation Professionals that live and work in the altitude see people who have lived in these places for long periods of time who have these conditions. They have acclimatized, so we need to know how best to use our tools to keep them safe, monitor and treat them, and most importantly, make them better. I hope this article was helpful you in providing those skills for your patients!
For more really cool stuff on altitude medicine, check out the “High Altitude Medicine and Biology” Journal. And I’m sending a big shoutout to my friend Nicole for requesting this topic!
Are you planning on traveling to a region of high altitude during the COVID-19 pandemic? Check out this guidance from the Mountain Medicine Association!
References
Center for Wilderness Safety. (2021). Oxygen at High Altitude. https://wildsafe.org/resources/outdoor-safety-101/altitude-safety-101/oxygen-levels-altitude/
Gallagher, S.A., & Hackett, P. (2021, July 14). Acute mountain sickness and high altitude cerebral edema. UpToDate. https://www.uptodate.com/contents/acute-mountain-sickness-and-high-altitude-cerebral-edema
The International Mountaineering And Climbing Federation (Union Internationale Des Associations D’Alpinisme). (2021). Advice and Recommendations Library. https://www.theuiaa.org/mountain-medicine/medical-advice/
Luks, A. M., & Swensen, E. R. (2011). Pulse Oximetry at High Altitude. High Altitude Medicine & Biology, 12(2). http://dev.amga.com/wp-content/uploads/2013/09/LuksSwensonPulseOximetryatHighAltitude.pdf
Meijer, H.J. & Jean, D. (2008). Consensus statement of the UIAA Medical Commission (Vol 9): Children at Altitude. The International Mountaineering And Climbing Federation (Union Internationale Des Associations D’Alpinisme). https://www.theuiaa.org/documents/mountainmedicine/UIAA_MedCom_Rec_No_9_Children_at_Altitude_2008_V1-1.pdf
Napier, P. J., & West, J.P. (1996). MMA Memo No 162: Medical and physiological considerations for high altitude. National Radio Astronomy Observatory. https://legacy.nrao.edu/alma/memos/html-memos/alma162/memo162.html
Paralikar S. J. (2012). High altitude pulmonary edema-clinical features, pathophysiology, prevention and treatment. Indian journal of occupational and environmental medicine, 16(2), 59–62. https://doi.org/10.4103/0019-5278.107066
Yesalis, C. E., & Bahrke, M. S. (2002). “History of Doping in Sport” (PDF). International Sports Studies, Vol 24, Issue 1. 2002. Archived from the original (PDF) on November 23, 2017.

Follow @DoctorBthePT on Twitter for regular updates!






